"Millions of people suffer needlessly from agonizing pain because physicians have been reluctant to use ‘high-risk’ opioids" A major problem faced by narcotics users and abusers is the well-known development of tolerance when an opiate is given repeatedly over a period of time. This is directly responsible for a number of the problems associated with narcotic use and abuse since increasing tolerance requires that steadily larger doses be used to achieve the same effects or degree of pain relief.
Crain & Shen 2000"The first thing they told us in medical school is that no one has ever died from pain but plenty of physicians have had their careers destroyed trying to help people who are in pain."
Comment from an emergency room physician requesting anonymity (2001)
Tolerance, Addiction and Effective Pain Management
some thoughts by K.TroutThis also underlies much of the crime associated with street addiction as the cost of maintaining a habit also escalates along with the dosage, often leading addicts to turn to drug dealing, prostitution or criminal activities to enable them to afford their daily dose.
Many experienced junkies, especially if heroin users, address this problem by taking regular breaks from their drug of choice, allowing their tolerance to diminish and their effective dosage to also be decreased. Due to the unpredictable quality of unregulated black-market street drugs this can actually be potentially dangerous if they then acquire material of greater potency than they were expecting. (Junkies who relapse after recovery face a similar risk when they return to use.)
Some users employ materials like cimetidine (Tagamet) [R.A.H. 2000] to retard drug metabolism and thereby maximize their effectiveness. [An interesting but unrelated point worthy of further investigation is the report of Peterson et al. 1983 indicating that use of cimetidine one hour before and after administration of large amounts of cocaine to rodents prevented hepatic toxicity and liver damage. Pellinen et al. 1994 also reported a prevention of “metabolism-related hepatotoxicity” by use of Cytochrome P450 3A inhibitors.]
Other users recommend grapefruit juice (Anonymous 2000) to interfere with the metabolism of the opiates by the liver and small intestinal Cytochrome P450 enzyme CYP3A and thus attempt to maximize their per dose effects, blood concentration and duration. While this has been reported by many users to be effective at maximizing per dose results this does not affect the development of tolerance.
Presently many questions remain, as there is also been some conjecture made that administration of grapefruit juice might interfere with the conversion of codeine to morphine due to its lesser inhibition of some CYP subfamilies. This does not seem to be the case; Caraco et al. 1996 reported (in animals) that if codeine was coadministered with selective inhibitors of CYP3A4 this could result in increased morphine production and enhanced effects due to “shunting into the CYP2D6 pathway” (as CYP2D6 would NOT be affected).
It is worth noting that I can thus far locate NOTHING in the *scientific* literature specifically supporting the use of grapefruit juice to increase the general effectiveness of opiates or even that CYP3A is responsible for the metabolism of heroin. Although, it is certainly reasonable to assume that CYP3A is responsible for its metabolism since it is proven as such for other opioids such as codeine (Caraco et al. 1996) and fentanyl (Feierman & Lasker 1996)
Reports of successful application, circulating orally among users (Anonymous 2000 & 2001) and posted on web-based bulletin boards, are common enough that this should be investigated further.
It is important to keep in mind that grapefruit juice can also prove problematic due to the elevated levels of bioavailable drug, requiring a reduction of the dosage. Sometimes it can even be dangerous if certain other drugs are being used. The combination of grapefruit juice with some specific pharmaceuticals has produced many serious problems and even some deaths. (Ameer & Weintraub 1997; Dresser et al. 2000)
Another practice reportedly employed by some narcotic users is combining hydroxyzine with opiates to potentiate their effects. This is said to produce a rough doubling of intensity with the addition of unwanted side effects like a dry mouth. [Anonymous 2000] It appears to have no effect on the development of tolerance.
An interesting approach is the combination of opiates with the opiate antagonists naloxone or naltrexone in miniscule amounts. The combination of less than 0.001% of what would be a normal dose of the antagonist with an opiate allows a far greater response (“at least 50%”) to the opiate which in turn permits a much lower effective dose to be used. It is also said to prevent respiratory depression, tolerance and addiction. This approach has apparently been patented (Crain & Shen 1996) and is being commercially developed by Pain Therapeutics. [R.A.H. 2000; Crain & Shen 2000]
Another interesting comment was made by Karl Jansen (2001) concerning the administration of small oral doses of ketamine being found to be of use in chronic pain clinic for “greatly reducing” the development of tolerance (via blockade of NMDA receptors).
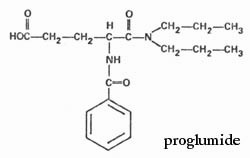
However, many people are unaware that both enhanced effectiveness of narcotic analgesics AND prevention or reversal of tolerance is readily achievable through the oral use of up to 200-250 mg of Proglumide [(DL)-4-Benzamido-N,N-dipropylglutaramic acid]. [See Ott 1999; Watkins et al. 1984]
The work of Watkins suggests there may be a therapeutic dosage window with diminished results above it but more detailed work to define this is apparently lacking.
Rather than simply augment the action of the opiates, proglumide actually interferes with the anti-opioid activity of the neuropeptide CCK.
The chronic administration of opiates, or spinal cord and other CNS injuries, elevates the level of Cholecystokinin (CCK) that is present. Such elevated levels exert an antagonistic effect on opioid activity resulting in significantly diminished analgesic effects. (Watkins et al. 1984; Xu et al. 1993 & 1994)
It is this rise in CCK levels that directly leads to the condition known as drug tolerance and the corresponding increase in its anti-opioid activity that requires the opiate user to use increasingly larger amounts to achieve the same effects.
This anti-opiate effect can be prevented or even reversed through the administration of CCK inhibitors such as proglumide. (Watkins et al. 1984)
Besides just interfering with the adverse action of CCK on opiate activity, proglumide is also known to augment the analgesic effect of opiates. Often this can provide a higher quality of analgesia for those patients who suffer from an incomplete response to pain medications.
Watkins & coworkers reported that proglumide reversed morphine tolerance and also 1) hastened the onset of analgesia, 2) increased the peak levels, and 3) prolonged the duration.
They suggested that not simply did this indicate that effective narcotic doses could be decreased but it also indicated that proglumide might be able to enhance the effects of other procedures, such as acupuncture, which involve endogenous opiates. (Watkins et al. 1984)
Proglumide is a nonselective CCK inhibitor that was formerly employed as an anti-ulcer medication (Hahne et al. 1981). It shows NO analgesic effects of its own.
Although proglumide is now considered to be an obsolete pharmaceutical due to changes in our understandings of ulcer etiology, it has already seen extensive pharmacological and toxicological testing proving its safety and has been approved for use in humans.
It has largely fallen into disuse but is still available in bulk via chemical houses or as a pharmaceutical in Europe and Africa sold under the trade name Milid and Milide.
Other CCK inhibitors show similar properties (Idänpään-Heikkilä et al. 1997; Xu et al. 1993). However, beyond simply having seen previous use in humans, proglumide is both inexpensive and nontoxic. (Ott 1999)
Proglumide is not some sort of magic bullet for completely eliminating the risk of tolerance development and addiction as its effects are only effective for a limited duration before tolerance to IT begins to develop. (After 8 days its effectiveness begins to wane) The work of Kellstein & Mayer 1990 suggests that successful therapeutic/maintenance applications will probably require its discontinuation for a week after each week of use. More work is needed to better define the precise parameters of its effective use for this purpose.
Despite this, proglumide has already demonstrated itself to be of value both in pain management and as an adjunct to maintaining a narcotic addiction within a larger program of harm reduction (Anonymous 2000; Ott 1999).
What is fascinating is how few drug educators, drug treatment facilities or even drug users are aware of this despite it being readily available information for nearly 20 years.
If development of tolerance and the high price of a sustained addiction are truly as serious of a problem as we all agree that they are, one can only wonder how it is that, despite the tools existing to remove or at least reduce this problem, there seems to be no interest or research except on a limited scale related to specific small areas of chronic pain management and understanding.
The current misguided approach of substituting methadone is commonly reported to actually cause MORE perceptual and thinking problems than the opiates it replaces PLUS methadone is known to cause physical damage to internal organs that are not encountered with opiate use itself.
Harm reduction approaches would benefit greatly by using proglumide as a cornerstone and making it readily available to both narcotic users and abusers.
Those who will most certainly object include organized crime and drug dealers who enjoy the obscene profits reaped from escalating drug tolerances, and possibly also the so-called “drug educators” that sadly often seem to be the ones most in need of some factual education.
There are many problems associated with opiate use and abuse. While the majority of these are legal in origin, the most sensible approach would be to ameliorate [or mitigate] those that aren’t.
Increased analgesic effectiveness and prevention of tolerance are two obvious areas where harm reduction is readily possible TODAY. Both sufferers of chronic pain and narcotic addicts stand to benefit from having their needs met and their health risks simultaneously decreased.
As this is first and foremost a health problem, the current approach of harm maximization is both counterproductive and unacceptable. To a rationale or caring mind it might even be perceived of as unethical and amoral.
Not only do sufferers of chronic pain and narcotic addicts stand to benefit from such harm reduction approaches but, by decreasing drug-associated crimes, a significant area of the true “drug problem” can be directly addressed, thereby benefiting society as a whole.
References:
Ameer, Barbara & Randy A. Weintraub (1997) Clinical Pharmacokinetics 33 (2): 103-121. “Drug Interactions with Grapefruit Juice.”Anonymous (2000 & 2001) Personal interviews with assorted opiate users & abusers.
Caraco, Y. et al. (1996) Drug Metab. Dispos. 24(7): 761-764. “Microsomal codeine N-demethylation: cosegregation with cytochrome P4503A4 activity.” [Y. Caraco, T. Tateishi, F.P. Guengerich & A.J. Wood] [Abstract from PubMed]
Crain & Shen 1996: See patent references farther below.
Crain, Stanley M. & Ke-Fei Shen (2000) Pain 84: 121-131. “Antagonists of excitatory opioid receptor functions enhance morphine’s analgesic potency and attenuate opioid tolerance/dependence liability.”
Dresser, G.K. et al. (2000) Clinical Pharmacokinetics 38(1): 41-57. “Pharmacokinetic-Pharmacodynamic Consequences and Clinical Relevance of Cytochrome P450 3A4 Inhibition.” [George K. Dresser, J. David Spence & David G. Bailey]
Entheogen Review; POBox 19820, Sacramento, CA 95819-0820. [www.entheogenreview.com]
Feierman DE, & J.M. Lasker (1996) Drug Metab. Dispos. 24(9):932-939. “Metabolism of fentanyl, a synthetic opioid analgesic, by human liver microsomes. Role of CYP3A4.” [Abstract from PubMed]
Hahne, W.F. et al. (1981) Proceedings of the National Academy of Science (USA) 78 (10): 6304-6308. “Proglumide and benzotript: Members of a different class of cholecystokinin receptor antagonists.” [W.F. Hahne, R.T. Jensen, G.F. Lemp & J.D. Gardner]
Idänpään-Heikkilä, J.J. et al. (1997) Journal of Pharmacology and Experimental Therapeutics 282 (3): 1366-1372. “Prevention of Tolerance to the Antinociceptive Effects of Systemic Morphine by a Selective Cholecystokinin-B Receptor Antagonist in a Rat Model of Peripheral Neuropathy.” [Juhana J. Idänpään-Heikkilä, Gisèle Guilbaud & Valérie Kayser]
Jansen, Karl (2001) e-mail correspondence with Jon Hanna (Book reference is to Ketamine: Dreams & Realities by Karl Jansen; see www.maps.org)
Kellstein, David E. & David J. Mayer (1990) Brain Research 516: 263-270. “Chronic administration of cholecystokinin antagonists reverses the enhancement of spinal morphine analgesia induced by acute pretreatment.”
Ott, Jonathan (1999) Entheogen Review 7(2): 62-73. “Jonathan Ott Speaks…Part Two.” (Interviewed by Will Beifuss & Jon Hanna in 1998) (Proglumide comments are on p. 69)
Pain Therapeutics, Inc., 250 E. Grand Avenue, STE 70, San Francisco, CA 94080
Peterson, F.J. et al. (1983) Gastroenterology 85(1): 122-129. “Prevention of acetaminophen and cocaine hepatotoxicity in mice by cimetidine treatment.” [F.J. Peterson, R.G. Knodell, N.J. Lindemann & N.M. Steele] [Abstract from PubMed]
Pellinen, P. et al. (1994) Eur. J. Pharmacol. 270(1): 35-43. “Cocaine N-demethylation and the metabolism-related hepatotoxicity can be prevented by cytochrome P450 3A inhibitors.” [P. Pellinen, P. Honkakoski, F. Stenback, M. Niemitz, E. Alhava, O. Pelkonen, M.A. Lang & M. Pasanen] [Abstract from PubMed]
R.A.H. (2000) Entheogen Review 9(3): 145-147. “Opiate Potentiation.”
Watkins, L.R. et al. (1984) Science 224: 395-396. “Potentiation of Opiate Analgesia and Apparent Reversal of Morphine Tolerance by Proglumide.” [L.R. Watkins, I.B. Kinscheck & D.J. Mayer]
Xu, X.-J., et al. (1993) Neuroscience Letters 152: 129-132. “Up-regulation of cholecystokinin in primary sensory neurons is associated with morphine insensitivity in experimental neuropathic pain in the rat.” [X.-J. Xu, M.J.C. Puke, V.M.K. Verge, Z. Wiesenfeld-Hallin, J. Hughes & T. Hökfelt]
Xu, X.-J., et al. (1994) Pain 56: 271-277. “Chronic pain-related behaviors in spinally injured rats: evidence for functional alterations of the endogenous cholecystokinin and opioid systems.” [Xiao-Jun Xu, Jing-Xia Hao, Åke Seiger, John Hughes, Tomas Hökfelt & Zsuzsanna Wiesenfeld-Hallin]
Additional information that was not used or referenced above:
CCK activity as opioid antagonist Faris, P.L. et al. (1983) Science 310-312. “Evidence for the neuropeptide cholecystokinin as an antagonist of opiate analgesia.” [P.L. Faris, B.R. Komisaruk, L.R. Watkins & D.J. Mayer]
(See also CCK inhibitor references below),Itoh, S. et al. (1982) Eur. J. Pharmacol. 80: 421-425. “Caerulein and cholecystokinin suppress B-endorphin-induced analgesia in the rat.” [S. Itoh, G. Katsuura & Y. Maeda]
Nichols, M.L. et al. (1995) J. Pharmacol. Exp. Ther. 275: 1339-1345. “Regulation of morphine anti allodynic efficacy by cholecystokinin in a model of neuropathic pain in rats.” [M.L. Nichols, D. Bian, M.H. Ossipov, J. Lai, & F. Porreca]
Wiesenfeld-Hallin, Z. & X-J. Xu (1996) Regulatory Peptides 65: 23-28. “The role of cholecystokinin in nociception, neuropathic pain and opiate tolerance.”
CCK inhibitors enhancing opioid analgesia and/or preventing tolerance Dourish, C.T. et al. (1988) Eur. J. Pharmacol. 147: 469-472. “Enhancement of morphine analgesia and prevention of morphine tolerance in the rat by the cholecystokinin antagonist L-364,718.” [C.T. Dourish, D. Hawley & S.D. Iversen]Dourish, C.T. et al. (1990) Eur. J. Pharmacol. 176: 35-44. “The selective CCK-B antagonist L-365,260 enhances morphine analgesia and prevents morphine tolerance in the rat.” [C.T. Dourish, M.F. O’Neill, J. Coughlan, S.J. Kitchener, D. Hawley & S.D. Iversen]
Hoffmann, O. & Z. Wiesenfeld-Hallin (1994) Neuro. Report 5: 2565-2568. “The CCK-B receptor antagonist CI 988 reverses tolerance to morphine in rats.”
Hughes, J. et al. (1990) Proceedings of the National Academy of Science (USA) 87: 6728-6732. “Development of a class of selective cholecystokinin type B receptor antagonists having potent anxiolytic activity.” [J. Hughes, P. Boden, B. Costall, A. Domeney, E. Kelly, D.C. Horwell, J.C. Hunter, R.D. Pinnock & G.N. Woodruff]
O’Neill, M.F. et al. (1989) Neuropharmacology 28: 243-249. “Morphine-induced analgesia in the rat paw is blocked by CCK and enhanced by the CCK antagonist MK-329.” [M.F. O’Neill, C.T. Dourish & S.D. Iversen]
Watkins, L.R. et al. (1985) Brain Research 327: 181-190. “Cholecystokinin antagonists selectively potentiate analgesia induced by endogenous opiates.” [L.R. Watkins, I.B. Kinscheck, E.F.S. Kaufman, J. Miller, H. Frenk & D.J. Mayer]
Wiesenfeld, Z. et al. (1990) Proceedings of the National Academy of Science (USA) 87: 7105-7109. “PD134308, a selective antagonist of cholecystokinin type-B receptor, enhances the analgesic effect of morphine and synergistically interacts with intrathecal galanin to depress spinal nociceptive reflexes.” [Z. Wiesenfeld, X.-J. Xu, J. Hughes, D.C. Horwell & T. Hökfelt]
Xu, X,-J. et al. (1992) British Journal of Pharmacology 105: 591-596. “CI988, a selective antagonist of cholecystokinin type-B receptor, prevents morphine tolerance in the rat.” [X.-J. Xu, Z. Wiesenfeld-Hallin, J. Hughes, D.C. Horwell & T. Hökfelt]
Grapefruit juice Bailey, D.G. et al. (1998) British Journal of Clinical Pharmacology 46(2): 101-110. “Grapefruit juice-drug interactions.” [David G. Bailey, J. Malcolm, O. Arnold & J.David Spence]Edwards, D.J. et al. (1996) Drug Metab. Dispos. 24(12): 1287-1290. “Identification of 6',7'-dihydroxybergamottin, a cytochrome P450 inhibitor, in grapefruit juice.” [D.J. Edwards, F.H. Bellevue III & P.M. Woster] [Abstract from PubMed]
Fuhr, U. (1998) Drug Safety 18(4): 251-272. “Drug interactions with grapefruit juice. Extent, probable mechanism and clinical relevance.” [Abstract from PubMed]
He, K. et al. (1998) Chem. Res. Toxicol. 11(4): 252-259. “Inactivation of cytochrome P450 3A4 by bergamottin, a component of grapefruit juice.” [K. He, K.R. Iyer, R.N. Hayes, M.W. Sinz, T.F. Woolf & P.F. Hollenberg] [Abstract from PubMed]
Tirillini B. (2000) Fitoterapia 71: S29-S37. “Grapefruit: the last decade acquisitions.” [Abstract from PubMed]
Naloxone, naltrexone & nalmefene enhancing morphine analgesia Bergman, St.A. et al. (1988) Arch. Int. Pharmacodyn. 291: 229-237. “Low dose naloxone enhances buprenorphine in a tooth pulp antinociceptive assay.” (St.A. Bergman, R.L. Wynn, D.E. Myers & F.G. Rudo]
and/or attenuating tolerance and dependenceCrain, S.M. & K.-F. Shen (1995a) Proceedings of the National Academy of Science (USA) 92: 10540-10544. “Ultra-low concentrations of naloxone selectively antagonize excitatory effects of morphine on sensory neurons, thereby increasing its antinociceptive potency and attenuating tolerance/dependence during chronic cotreatment.”
Crain, S.M. & K.-F. Shen (1996) US Patent No. 5,512,578, US Patent Office. “Method of simultaneously enhancing analgesic potency and attenuating dependence liability caused by exogenous and endogenous opioid agonists.”
Crain, S.M. & K.-F. Shen (1996) US Patent No. 5,580,876, US Patent Office. “Method of simultaneously enhancing analgesic potency and attenuating dependence liability caused by morphine and other bi-modally-acting opioid agonists.”
Crain, S.M. & K.-F. Shen (1998b) Trends Pharmacol. Sci. 19: 358-365. “Modulation of opioid analgesia, tolerance and dependence by Gs-coupled, GM1 ganglioside-regulated opioid receptor functions.”
Gan, T.J. et al. (1997) Anethesiology 87: 1075-1081. “Opioid-sparing effects of a low-dose infusion of naloxone in patient-administered morphine sulfate.” [T.J. Gan, B. Ginsberg, P.S.A. Glass, J. Fortney, R. Jhaveri & R. Perno]
Gillman, M.A. & F.J. Lichtigfeld (1985) Neurol. Res. 7: 106-119. “A pharmacological overview of opioid mechanisms mediating analgesia and hyperalgesia.” (Review)
Gillman, M.A. & F.J. Lichtigfeld (1989) Int. J. Neurosci. 48: 321-324. “Naloxone analgesia: an update.” (Review)
Holmes, B.B. & J.M. Fujimoto (1993) Anesth. Analg. 77: 1166-1173. “Inhibiting a spinal dynorphin A component enhances intrathecal morphine antinociception in mice.”
Joshi, G.P. et al. (1999) Anesthesiology 90: 1007-1011. “Effects of prophylactic nalmefene on the incidence of morphine-related side effects in patients receiving intravenous patient-controlled analgesia.” [G.P. Joshi, J. Duffy, J. Chehade, J. Wesevich, N. Gajraj & E.R. Johnson]
Levine, J.D. et al. (1988) J. Clin. Invest. 82: 1574-1577. “Potentiation of pentazocine analgesia by low-dose naloxone.” [J.D. Levine, N.C. Gordon, Y.O. Taiwo & T.J. Coderre]
Shen, K.-F. & S.M. Crain (1997) Brain Research 757: 176-190. “Ultra-low doses of naltrexone or etorphine increase morphine’s antinociceptive potency and attenuate tolerance/dependence in mice.”
Proglumide Chiodo, L.A. & B.S. Bunney (1983) Science 219: 1449-1450. “Proglumide, selective antagonism of excitatory effect of cholecystokinin in central nervous system.”Katsuura, G. & S. Itoh (1985) Eur. J. Pharmacol. 107: 363-366. “Potentiation of ß-endorphin effects by proglumide in the rat.”
Lavigne, G. et al. (1987) Pain, Suppl. 4: S229. “Potentiation of morphine analgesia by proglumide for acute clinical pain.” [G. Lavigne, K.M. Hargreaves, G.P. Miller, E.S. Schmidt & R.A. Dionne]
McCleane, G.J. (1998) Anesth. Anal. 87: 1117-1120. “The cholecystokinin antagonist proglumide enhances the analgesic efficacy of morphine in humans with chronic benign pain.”
McCleane, G.J. (1998) The Pain Clinic 11: 103-107. “The cholecystokinin antagonist proglumide enhances the analgesic effect of morphine in chronic benign nociceptive and neuropathic pain.”
Rovati, L.C. et al. (1985) Annals of the New York Academy of Science 448: 630-632. “Effects of proglumide on morphine analgesia and tolerance.” [L.C. Rovati, P. Sacerdote & A.E. Panerai]
Tang, J. et al. (1984) Neuropharmacology 23 (6): 715-718. “Proglumide prevents and curtails acute tolerance to morphine in rats.” [J. Tang, J. Chou, M. Iadarola, H.-Y.T. Yang & E. Costa]
Watkins, L.R. et al. (1985) Brain Research 327: 169-180. “Potentiation of morphine analgesia by the cholecystokinin antagonist proglumide.” [L.R. Watkins, I.B. Kinscheck & D.J. Mayer]
E-mail: K Trout
trout@opioids.wiki
HOME
Glossary
Opium Images
Pain medication online
The Birth of a New Generation